Diabetes is a growing condition throughout the world, affecting rich and poor alike. Costing Australians more than $6 billion each year, there are enormous implications for our health-care system. Our collection of articles and guides can help you recognise the signs and symptoms, manage and monitor pre-existing conditions, and most importantly, help prevent it in the first place.
Diabetes
Diabetes
Knowing the causes of diabetes is as important as knowing how to treat it.
Review and compare
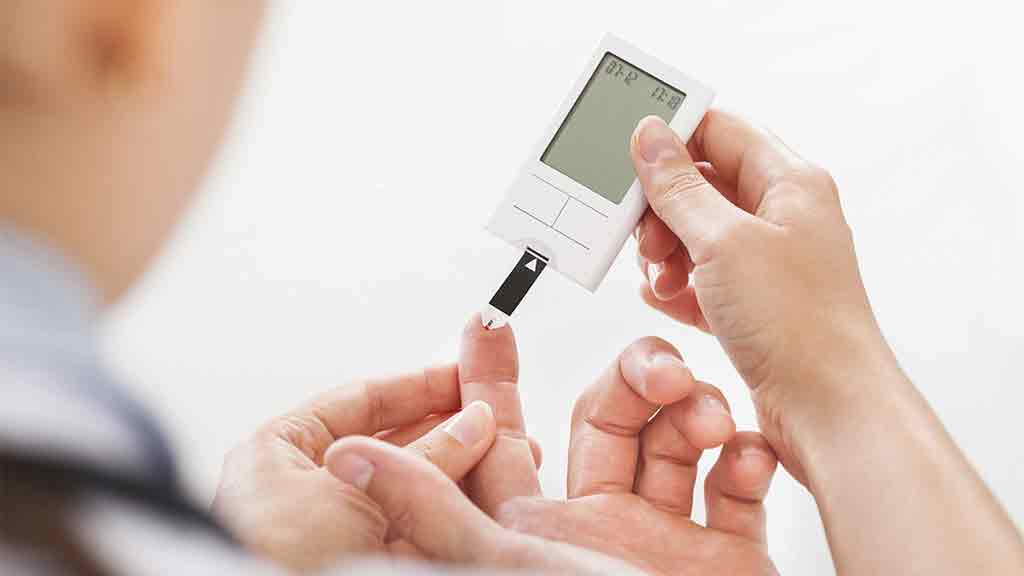
Blood glucose meter reviews
We test blood glucose meters including models from Accu-Chek, CareSens, Trueresult and more.
Buying guides
How to buy the best blood glucose meter
If you're a person with diabetes you'll understand the importance of having a reliable device on hand.
Articles