Varicose vein treatments
If you're suffering from varicose veins, it's good to know they can be treated effectively with minimal discomfort. But it's important to review your options.
Last updated: 16 Sep 2021
Varicose veins aren’t just a cosmetic problem. They can also cause a fair amount of pain and discomfort on a daily basis, with some of the more persistent symptoms including swelling, throbbing and leg cramps. Serious complications can develop over time too, such as phlebitis (vein inflammation), blood clots, dermatitis and painful vein ulcers that, in extreme cases, can lead to amputation.
Many forms of treatments exist to suit individual cases, personal preferences and budgets. One of the newer treatments on the market is endovenous laser therapy – a less invasive alternative to surgery performed by experienced and skilled practitioners, with good success rates reported
In this article we explain what varicose veins are, who gets them, and what treatment options are available, as well as management strategies to help reduce discomfort.
What are varicose veins?
There are two venous systems in our legs – deep veins and superficial veins – which are connected by smaller perforator veins. Most varicosities are a result of problems with the main superficial, or saphenous, veins that collect blood from other surface veins.
One-way valves in veins direct the flow of blood back to the heart. In the legs – the most common site of varicose veins – these valves are particularly important because the blood is flowing against gravity. When one or more valves fail, blood can pool in the section, causing the bulgy, tortuous appearance of varicose veins. Weak vein walls also make the problem worse.
When the blood flows backwards because of weak valves, it’s known as reflux. Deeper veins, which lie within and between muscles, aren’t affected in the same way, because muscular contraction (when walking and so on) compresses the veins, creating a pumping action that returns blood to the heart and provides support. The veins near the surface, however, have very little support overall.
Not all varicosities are caused by problems in the saphenous or perforating veins though; any superficial leg vein can become varicose, although these lesser veins are usually quite small and cause few symptoms. However, the severity of the symptoms isn’t always related to the appearance of the veins, and even large, obvious ones may cause little or no discomfort.
Varicose veins serve no useful purpose; alternative pathways have already been formed to bypass the abnormal varicose veins and return blood to the heart. Compressing, closing off or eliminating varicose veins improves circulation and relieves many of the symptoms.
Who gets varicose veins and why?
In Western nations it’s estimated about 40% of people suffer from varicose veins, and it appears to be hereditary. Susceptibility varies among cultures, although it’s not clear if this is genetic or lifestyle-related (poor diet and lack of physical activity may be partly responsible).
Women seem to get varicose veins more than men, probably because of the hormone oestrogen. Taking oestrogen-based contraceptive pills or hormone replacement therapy also appears to increase risk. Women who have had children are more likely to get varicose veins in the future, as hormones released during pregnancy relax vein walls, and the weight of the baby puts more pressure on leg veins. Varicose veins that occur during pregnancy often go away within a few months of giving birth though.
Poor diet, obesity, smoking and a sedentary lifestyle increase risk, as does standing still for long periods of time.
Getting treatment
As there’s no cure for varicose veins, there’s also no guarantee that one treatment will fix the problem for life. The earlier you treat varicose veins though, the more successful the outcome will be.
Your first port of call should be your GP, who can refer you to a phlebologist, vascular specialist or other surgeon who practises phlebology (the diagnosis and treatment of venal disorders). An ultrasound “map” of your blood vessels will provide an overview of how they’re functioning and where the problems lie, and can give you insight into what the future holds if you choose to do nothing.
Treatment may require several stages. For severe cases, the first stage is usually to treat the root of the problem – the saphenous veins. The reflux in these veins affects the tributary veins that run from them. Once the saphenous veins have been fixed, secondary incidences can then be treated. Spider veins are almost always associated with deeper vein problems, so further investigation is needed to identify the cause (which should then be treated first).
Most treatments are done in an office or clinic setting with local or no anaesthetic. Ligation and stripping takes place in hospital and may require general anaesthetic.
After any treatment, patients have to wear compression stockings day and night for about two weeks to help in sealing veins and preventing clots. Regular walking is an important part of healing too, though you may have to avoid more strenuous exercise for a while. Your physician will perform an ultrasound soon after the treatment to ensure there are no clots.
Managing varicose veins without surgery
If your varicose veins aren’t too severe, or you’re trying to slow down their recurrence, the following strategies may help:
- Regular exercise, a low-fat diet with plenty of fruit and vegetables, and keeping your weight at a healthy level can help prevent varicose veins becoming a problem.
- Elevating your legs when possible can provide relief, as can compression stockings, which are elastic stockings that use graduated pressure to squeeze your veins and stop blood from pooling or flowing backwards.
- Clinical trials of horse chestnut tablets found the naturally-occurring chemical, aescin, reduced pain, itching and swelling, at least in the short term. It appears to be safe, although it may interact with some medicines (check with your doctor), and its long-term effectiveness hasn’t been established.
- Some cosmetic creams claim to reduce the appearance of spider veins, but there’s no evidence they have anything more than a minor effect.
Procedures, risks and costs
Microsclerotherapy and ultrasound-guided sclerotherapy
An irritating liquid or foam is injected into the blood vessel, causing it to swell and stick together, aided by external pressure from compression stockings. The blood vessel is eventually absorbed by surrounding tissue and fades. This treatment is often used together with vascular ultrasound to guide the injections in larger and/or deeper veins.
Costs: Ultrasound-guided sclerotherapy costs about $800-$1000; sclerotherapy for small veins and spider veins is more like $300-$500.
Ambulatory phlebectomy
A tiny cut is made over the vein which, using a phlebectomy hook, is then pulled out until it breaks or cannot be pulled any further. The process is repeated along the entire length of the vein to be extracted, and no stitches are needed.
Costs: About $900.
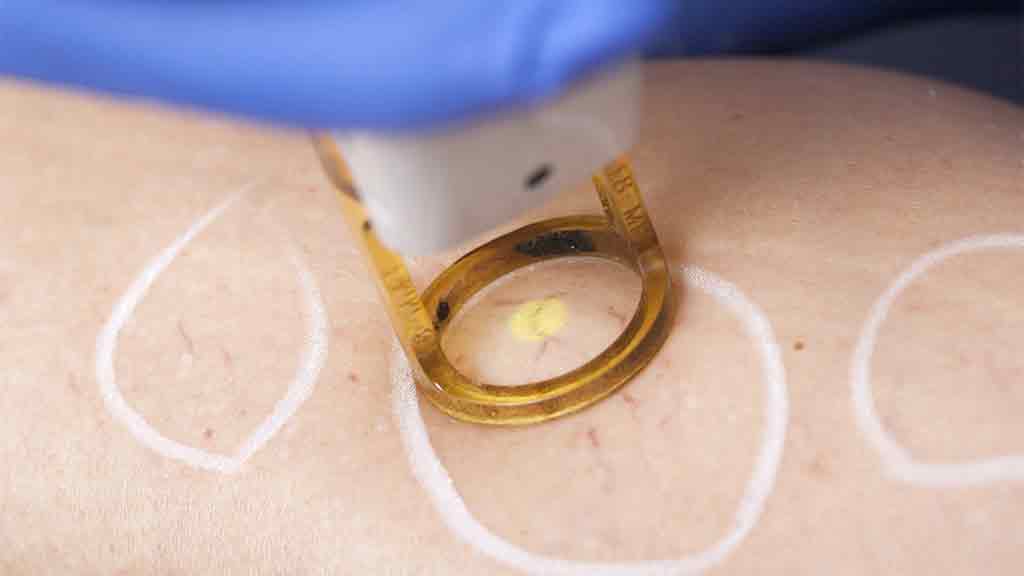
Endovenous laser therapy
This is one of the most recent treatments to become available. The vein is punctured near the knee or ankle, depending on which part of the vein is being treated, and a fine laser probe is inserted. The laser’s activated, causing the vein walls to close off as it’s withdrawn. The procedure involves some discomfort and local anaesthetic is used to reduce pain. This therapy may be used in conjunction with ultrasound-guided sclerotherapy.
Costs: Between $2500 and $4000 per treatment, depending on the scale of the problem. See below for more about endovenous laser therapy.
Radiofrequency ablation
Similar in technique and outcome to endovenous laser therapy, radiofrequency ablation uses a catheter to heat the blood and destroy the vein.
Costs: Costs and risks are similar to endovenous laser therapy.
Surgery
An incision is made at the top of the leg over the vein, which is then cut and tied off (ligation). A thin wire is then inserted down the length of the vein and the vein is pulled out (stripping). Smaller incisions may be needed to separate connecting veins along the way.
Costs: About $2000, plus hospital and anaesthetic costs.
Treatment risks
All types of treatment are likely to result in temporary bruising, aching, discolouration and inflammation. Deep vein thrombosis (DVT) and temporary numbness due to nerve damage are rare. For one treatment, sclerotherapy, additional but rare risks include pockets of blood trapped in veins (this is different from DVT), pigmentation along treated veins, allergic reaction to the solution and skin ulceration.
Costs and rebates
Medicare rebates apply to most procedures considered medically necessary, so your varicose vein treatment needs to be more than just a cosmetic concern, and veins should be 2.5mm or more in diameter and have reflux in order to be eligible for rebates. But the amount of the rebate can depend on the severity of the veins and your individual Medicare circumstances (i.e. your Safety Net Threshold). And any rebate will most likely only cover a fraction of the overall cost.
The costs we’ve provided are only a guide for comparative purposes. Your doctor can give you a more accurate guide to overall costs and any applicable rebates. Private health insurers don’t cover most treatments because it doesn’t take place in a hospital, but they may cover part of the cost of post-operative compression stockings.
Accreditation
Endovenous laser therapy isn’t cheap, and in the wrong hands it can be ineffective or even dangerous. If you’re undergoing endovenous laser therapy, it’s important to know the person performing the procedure is an accredited professional trained in its operation.
The machines are readily available, so in theory anyone could buy and use one. Although they’re expensive, some companies overseas are giving the machines away for free, relying on recouping their expenses from the high cost of consumables, such as the laser probes themselves. According to the Australasian College of Phlebology, this has led to sometimes disastrous results in the US, such as probes breaking off in the blood vessels (because they were used too often) and long-term complications from incorrect use by unqualified operators.
Vascular surgeon Professor Michael Grigg pointed out that a thorough diagnostic assessment takes more than just knowledge of the technique, which isn’t difficult to learn, but also a good understanding of vascular medicine. “We have a saying in surgery: it takes about three months to learn how to do a procedure, but it takes three years to learn when to do it.”
Whatever treatment is recommended for you, make sure the treating doctor is accredited by the appropriate professional body:
Accredited practitioners can be located via these websites:
Australasian College of PhlebologyAustralian and New Zealand Society of PhlebologyAustralian and New Zealand Society for Vascular SurgeryRoyal Australian and New Zealand College of Radiologists
Karina worked at CHOICE from 2000 to 2018, and continues to contribute as a freelancer, mostly on health and lifestyle matters.
You can find me on LinkedIn.
Karina worked at CHOICE from 2000 to 2018, and continues to contribute as a freelancer, mostly on health and lifestyle matters.
You can find me on LinkedIn.